Define intellectual disability.
A developmental condition characterised by global impariment of intelligence and significant difficulties in socially adaptive functioning.
E.g. The presence of:
- reduced ability to understand new or complex information or to learn new skills;
- less able to cope independently;
- impairment that started before adulthood, with a lasting effect on development.
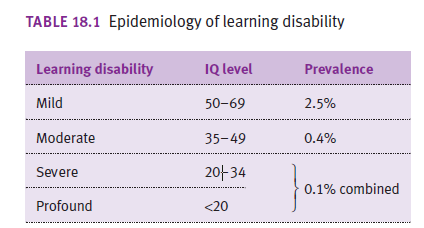
How common is ID?
- 2-3% prevalence
- Many never formally diagnosed
- F>M (3:2)
What is the aetiology of ID? List 2 antenatal, perinatal and postnatal causes of learning disability.
Usually no specific cause e.g. brain damage, genetic abnormalities, hypothyroidism. Multifactorial causes are common.
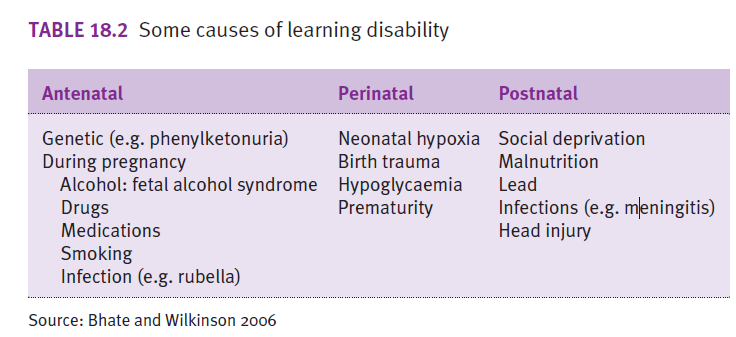

Name 3 syndromes associated with learning disability.
- Down syndrome
- Fragile X
- Fetal alcohol syndrome
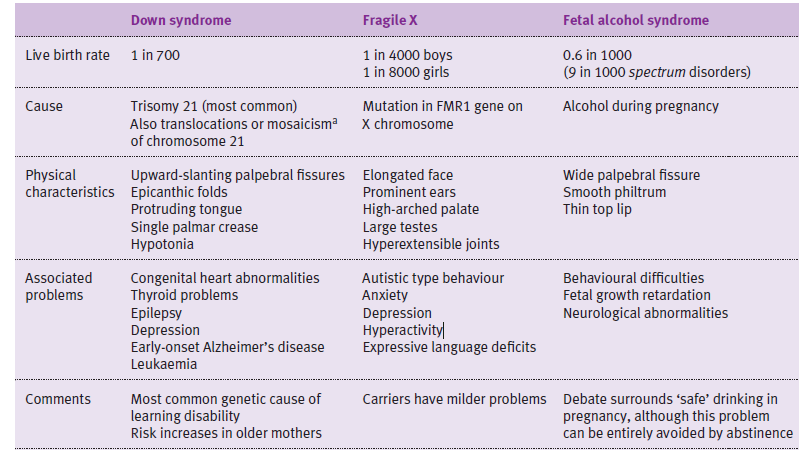
List 5 clinical features of learning disability.
Presents in childhood but can be missed if mild
Abilities in … are delayed /reduced /absent:
- language
- schooling
- motor ability
- independent living
- social ability
- employment
Behavioural difficulties - 2o to combination of
- communication problems
- psychiatric illness
- physical illness
- epilepsy
- suboptimal support
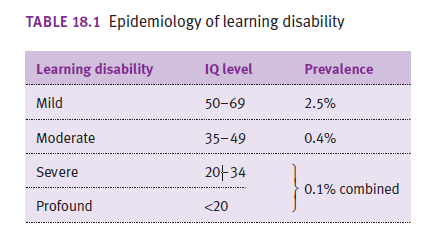
What are the levels of ID?
- Profound: <20
- Severe: 20-35
- Moderate: 35-50
- Mild: 50-69
List 2 features of each level of ID.
- Mild
- Language: usually good, but its development may be delayed
- Cognitive, motor, social: many live and work independently.
- Moderate
- Language and cognitive abilities: less developed.
- Motor and social: Reduced self-care abilities and limited motor skills +/- long-term supported accomodation. Simple practical work should be achievable in supported settings.
- Severe
- Motor: Marked impairment of motor function.
- Language: Little/no speech in early childhood
- Cognitive and social: Simple tasks performed with assistance. Likely to require their family home or 24-hourstaffed home.
- Profound learning disability
- Language, cognitive, social, motor: Severely limited language, communication, self-care, and mobility. Usually require higher levels of support.
- Significant associated medical problems.
What are the components of the Wechsler Adult Intelligence Scale?
2 main components:
Verbal scales: general knowledge, digit span, vocabulary, simple arithmetic, comprehension, similarities
Performance scale: picture completion, arrangement, block design, digit symbol, object assembly.
What are the differential diagnoses in ID?
ASD - in Asperger’s there may be significant social deficits, communication difficulties and daily living issues
Epilepsy - frequent uncontrolled seizures can mimic persistent cognitive impairment
Brain injury or progressive neurological conditions*
Psychiatric - schizophrenia if severe and persistent, can lead to chronic impairment across many domains
Educational disadvantage/neglect - lacking opportunity to learn must be distinguished from LD.
*learning disabilities are neurodevelopmental disorders, occurring while the brain is still developing. If the patient presents late, it is important to decide whether or not impaired intellect was present before any adult illness.
What psychiatric comorbidities are common in those with ID?
~30–50% of people with LD have additional mental health problems and associated autistic spectrum disorders.
- Schizophrenia (3%)
- Mood disorders (x4)
- Autism (75% of those diagnosed have ID)
What are the physical comorbidities commonly present in ID?
- Obesity and poor diet
- Epilepsy
- Sensory impairment e.g. hearing loss, poor visual acuity
- Infections - less likely to be screened or have vaccinations
How do you assess for ID?
- Intellectual impairment - assessed using the WAIS IV: 11 subtests to derive Verbal IQ + Performance IQ = Full Scale IQ
- Adaptive/Social functioning - established via clinical interview and ABAS II (Adaptive Behaviour Assessment System)
Presence in childhood established using clinical interview and school reports
What is the average score for the WAIS scale?
- Average Range: 70-130.
- Average score: 100
What additional investigations should be done for ID?
- IQ testing: is there global intellectual impairment?
- Functional assessment of skills, strengths and weaknesses.
- Detailed developmental history from parents, e.g. details of pregnancy and birth, language and motor skills development, schooling, emotional development, and relationships. School reports are helpful.
- FBC, U&E, LFT, TFT, bone profile—to exclude reversible disturbances.
- Additional blood tests for known causes of learning disability.
- Investigations for associated physical illnesses, e.g. EEG for epilepsy.
- Genetic testing if appropriate.
What condition causing ID do these patients have?
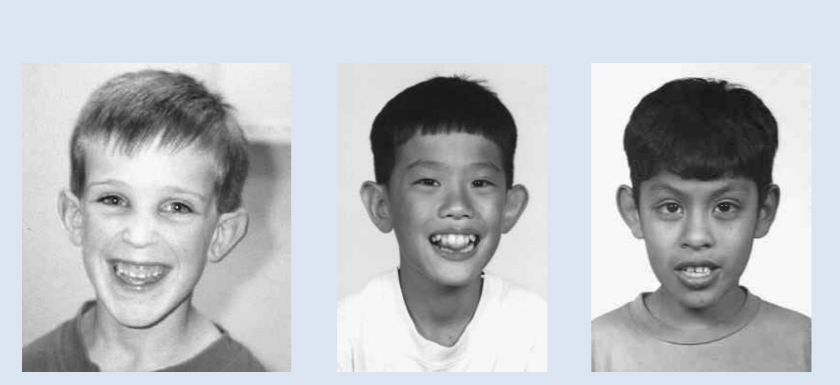
Fragile X
What are 3 steps taken to prevent learning disability?
- Parental Education (e.g. risks of alcohol during pregnancy)
- Improved antenatal/perinatal care
- Genetic counselling
- Early detection and treatment of reversible causes (e.g. excluding phenylalanine in babies with PKU)
What is the management of ID?
Biopsychosocial approach
Biological:
- Treat physical comorbidity
- Patients may be particularly sensitive to medications so slower dose titration and careful monitoring maybe required
Psychological:
- Treat psychiatric comorbidity - mental health problems can be difficult to diagnose because of cognitive, language and communication difficulties
- May include counselling, group therapy and modified CBT
- Behavioural therapy - helps improve unhelpful behaviour patterns + ABC approach
Social:
- Educational Support
- Statement of Special Educational Needs allow appropriate support
- This may be in mainstream or specialised schools
- The aim is to maximise the child’s potential
- Support network is needed to provide specific help with daily living, housing, employment and finances
- Assess carers’ needs
Describe the ABC approach used in behavioural therapy in ID.
ABC:
- Antecedents –> avoiding antecedents
- Behaviour –> reinforcing positive behaviours and preventing reinforcement of negative behaviours (e.g. using distraction techniques)
- Consequences –> helping people understand the consequences of their actions
What is the importance of the Equality Act (2010) in treatment of patients with ID?
People with learning disabilities to utilise mainstream services as much as is possible
Ensuring equity of access to health care for people with a learning disability is every health professional’s business.
Who is included in the community learning disability teams?
- Community learning disability nurses
- Psychiatrists
- Psychologists
- OT
- SALT
- Physiotherapists
- Dieticians
- Care managers
What tool can be used to promote normal daily living e.g. choice-making, in ID?
Choice board - with pictures; fosters sense of control and independance
Self-help board - helps service users learn new skills or activities; each picture is in order of the task
Schedule board calendar - provides structure to person’s day /life
Communication board - with emojis or emotions
Define adaptive functioning.
Performance in coping on a day-to-day basis with the demands of the environment and is related to age and socio-cultural expectancies.
What is diagnostic overshadowing?
The tendency to attribute everything to the learning disability itself
e.g. dismissing someone with LD who is crying and stops eating because ‘that’s the way these people are sometimes’—when appendicitis is the problem
What is challenging behaviour?
Culturally abnormal behaviour
Often persistent
Not a diagnosis


