Misc Flashcards
(120 cards)

COPS - 3977
Ciliary (3), Otic (9), Pterygopalatine (7), Submandibular (7)

What is a rolling and a sliding hernia?
Rolling - Gastroesophageal junction in place and gastric fundus herniates upwards
Sliding - Cardia of stomach herniates upwards into oesophagus

Where can an infection spread between the investing and visceral part of the pretracheal fascia?
inferiorly into the chest, causing infection of the anterior mediastinum.
Where can an infection Posterior to the prevertebral fascia spread?
Retropharyngeal space, down into mediastinal contents


At what spinal level do oyu palpate the carotid?
C6
What spinal level does the carotid bifurcate? What about trachea and aorta?
Carotid - C4
Trachea - T4
Aorta - L4
What nerve controls the dilator pupillae?
Sympathetic nervous system
What nerve controls sphincter pupillae?
Ciliary ganglion
What is the most common non trauma cause of facial paralysis? Where does it occur? What happens?
- Most common non trauma cause is inflammation of the facial nerve near its exit from the cranium at the stylomastoid foramen:
- Inflammation causes edema which compresses the nerve at the intracranial facial canal.
- Results in affected area sagging
What structure does the facial nerve pass through? Why is this clinically relevant? Where can disease of this structure refer to?
- Nerve passes through the parotid gland and therefore vulnerable to injury during surgery on the gland or disease of the gland:
- Parotid gland disease can cause pain in the temporal region and auricle of the ear.




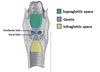
What are the green, orange, purple and red fascia in the pic?

Green - investing layer
Purple - Pretracheal layer
Orange - Prevertebral layer
Red - Carotid sheath

What is the platysma? Where is it found and what supplies it? What is its function?
- Broad thin sheet of muscle in the superficial cervical fascia.
- Supplied by the facial nerve
- Depresses the mandible and draws the corners of the mouth inferiorly.
Where can an infection spread:
a) between investing and muscular pretracheal
b) between investing and visceral pretracheal
c) between prevertebral and investing
a) cant spread beyond manubrium (superior part of sternum)
b) can spread into thoracic cavity anterior to pericardium
c) can spread laterally in the neck, may perforate fascial layer and enter retropharyngeal space resulting in a bulge in the pharynx and difficulty swallowing and speaking (dysphasia and dysphonia).
What is the borders of the anterior triangle of the neck?
Superiorly – Inferior border of the mandible (jawbone)
Laterally – Medial border of the sternocleidomastoid
Medially – Imaginary sagittal line down midline of body

What are the borders of the posterior triangle of the neck?
Anterior: Posterior border of the SCM.
Posterior: Anterior border of the trapezius muscle.
Inferior: Middle 1/3 of the clavicle.







What are the 4 types of cranial fractures? How does basal skull fracture present?
Depressed – Bone depresses inwards. Possible brain injury,
Linear – Break in bone traversing its full thickness. Most common.
Basal Skull – Affects base of the skull. Presents with bruising behind ears, known as ‘Battle’s sign’ or bruising around the eyes / orbits, known as Raccoon eye’s.
Diastatic – Fracture that occurs along a suture line causing a widening of the suture. Most often seen in children.


What are the features of cervical vertebrae?
- Triangular vertebral foramen
- Bifid spinous processes
- Transverse foramina