Hemodynamics 1 and 2 Flashcards
(37 cards)
Role of the Cardiovascular System (9)
- Move oxygen from the lungs to all body cells
- Move nutrients and water from the gastrointestinal system to all body cells
- Move metabolic wastes from all body cells to kidney for excretion
- Move heat from cells to skin for dissipation
- Move carbon dioxide from body cells to lungs for elimination
- Move particular toxic substances from some cells to liver for processing
- Move hormones from endocrine cells to their targets
- Move stored nutrients from liver and adipose tissue to all cells
- Carries immune cells, antibodies, and clotting proteins to wherever they are needed
Pulmonary vs. Systemic Circulation
- Pulmonary
- Right heart –> lungs
- Permit gas exchange (oxygenation of the blood and removal of CO2)
- Systemic
- Left heart –> body (except lungs)
- Perfuses all the cells of the body
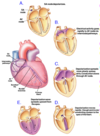
Anatomy of the Cardiovascular System
- Superior and inferior vena cava
- Blood is blue b/c carries less oxygen than blood in systemic circulation
- Right atrium
- Tricuspid valve
- Assures unidirectional blood flow
- Right ventricle
- Pulmonary semilunar valve
- Pulmonary arteries
- Lungs
- Blood is oxygenated
- Pulmonary veins
- Left atrium
- Bicuspid (mitral) valve
- Left ventricle
- Aortic semilunar valve
- Aorta
- Distributes oxygenated blood throughout body
What heart is enclosed in and mainly comprised of
- Heart is enclosed in a tough membranous sac: pericardium
- Heart is mainly comprised of cardiac muscle: myocardium
Matching of Pulmonary and Systemic Blood Flow
- Volume of blood leaving left and right heart per unit time must be matched
- Otherwise, fluid would accumulate in one system
- Ex. Severely damaged left ventricle (congestive heart failure)
- Blood would accumualte in pulmonary circulation
- –> impairment of gas exchange in the lungs
Blood
- Liquid medium: plasma
- 50-55% blood volume
- Contains plasma proteins (albumin, globulin), electrolytes, hormones, enzymes, and blood gases
- Formed elements
-
Red cells (erythrocytes)
- 40-45% total blood volume
- Centrifuged: settle to bottom
- Hematocrit: volume of RBCs in blood
- Contain hemoglobin: bind w/ & transport oxygen
-
White cells (leukocytes)
- 5% total blood volume
- Centrifuged: settle on top of red cells
- For immune processes & bodily defense
-
Platelets
- Little blood volume
- For blood coagulation
-
Red cells (erythrocytes)
Fluid Flow & Pressure
- Fluid moves form regions of higher pressure to regions of loewr pressure
- Contraction of ventricles imparts pressure
- Friction is lost as blood flows through blood vessels

Ohm’s Law
- ( Q = ΔP/R ) or ( ΔP = Q * R ) or ( R = ΔP/Q )
- ΔP = change in pressure on two ends of a vessel (not within the vessel itself)
- Q = blood flow
- R = resistance
- Flow through a vessel will be directly proportional to pressure and inversely proportional to resistance
- Ex. if you increase the length of a vessel, you increase resitance and decrease flow
Poiseuille’s Law
- Q = πΔPr4/ 8ηl
R = 8ηl / πr4- Q = flow
- π/8 is a constant
- ΔP = the pressure driving force
- r = radius of the vessel
- η = viscosity of the fluid
- l = length of the vessel
- Explains the flow of fluid through tubes of different sizes
- A change in radius has a huge effect on blood flow
- If halve the radius, you decrease blood flow by 16x
- Only valid under conditoins of laminar flow
Laminar vs. Turbulence / Tubulent Flow
- Laminar flow
- Fluid on the inside moves faster than the fluid on the outside of a vessel
- Large vessel: fluid flows faster
- Small vessel: fluid flows slower
- Ex. normal blood flow
- Turbulence
- As flow velocity increases, eventually a criticla velocity is reached at which the concentric layers break down
- –> side-to-side motion of fluid
- Increased turbulence –> increased viscosity –> decreased flow
- Turbulent Flow
- Frictional resistance is increased
- The bigger the vessel (increased diameter) and the quicker the blood flow (increased velocity), the more likely turbulent flow will occur
- Sounds which emanate from the circulatory system (murmurs) are the result of localized turbulence

Reynold’s Number (Re)
- Re = dvD/η
- d = fluid density
- v = velocity
- D = tube diameter
- η = viscosity
- Critical Re = 1000
-
Re < 1000 –> laminar flow
- Smaller vessels
- Decreased velocity
-
Re > 1000 –> turbulen flow
- Larger vessels
- Increased velocity
Poiseuille’s Law and Vasodilation/Vasoconstriction
- Can affect blood flow by altering blood vessel size via vasodilation/vasoconstriction
- Vasodilation –> decreased resistance –> increased blood flow
- Vasoconstriction –> increased resistance –> decreased blood flow

Poiseuille’s Law and Hematocrit
- Increased hematocrit –> increased viscosity –> increased resistance –> decreased blood flow
- Anemia: low hematocrit, increased blood flow
- Polycythemia: high hematocrit, decreased blood flow
Blood Pressure: Systole, Diastole, Pulse, Pulse Pressure
- Systole: cardiac muscle contracts
-
Diastole: cardiac muscle relaxes
- Lasts 2x as long as systole
- If heart rate = 67
- Cardiac cycle = 900 ms
- Diastole = 600 ms
- Systole = 300 ms
- Pulse: wave transmitted when the left ventricle contracts
-
Pulse pressure: amplitude of pulse wave
- Depends on the volume of blood ejected and the compliance of the arteries
Blood Pressure: Potential vs. Kinetic Energy
- Arteries contain fibrous and elastic connective tissue
- When high-pressure blood contacts arterial walls, potential energy is absorbed when the artery becomes stretched
- Energy is released as kinetic energy through elastic recoil
- Process limits the drop in arterial pressure during diastole
- Flow of blood from arteries to capillaries is continuous even though the flow from ventricle to aorta is pulsatile
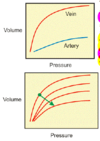
Compliance
- Tendency of a hollow organ to resist recoil toward its original dimensions
- Ability of an artery to absorb energy during systole and resorb it during diastole
- Ability of the arterial tree to store potential energy depends on compliance
- C = ΔV/ΔP or ΔP = ΔV/C
- ΔV = stroke volume
- ΔP = pulse pressure
- C = 0 –> completely rigid vessels
- –> all energy of contraction would be kinetic energy
- –> pressure would fluctuate: high during systole, low during diastole
Mean Arterial Pressure (MAP)
- Driving force for fluid entering arterial circulation
- Determined by measuring blood pressure continuously and determining the mean level
- Estimated from rmeasurements of systolic and diastolic BP
- Diastole lasts twice as long as systole
- MAP = 2/3 (diastolic P) + 1/3 (systolic P)
- Innacurate when HR becomes high b/c time spent in diastole decreases
- MAP = CO * TPR
- Based on ΔP = Q * R
- MAP = ΔP when pressure in the vena cava is assumed to be 0
- CO = Q = SV * contractions/time = SV * HR
- TPR = total peripheral resistance (sum of resistances provided by every arterial bed)
- R = total resistance in the cardiovascular system
Clinical Manifestations of Alterations in Vessel Properties
- Effects of smooth muscle vasoconstriction
- Nutrient delivery
- Myogenic autoregulation
- Advantages of increasing BP
- Compliance during aging
- Smooth muscle vasoconstriction –> increased BP –> decreased blood flow to downstream capillaries
- Deprives oxygen and nutrients from downstream tissues
- Nutrient delivery depends on blood flow through the capillary bed perfusing tissue
- Myogenic autoregulation: nromalizes blood flow as pressure changes so only large changes in pressure –> changes in tissue perfusion
- Advantages of increasing BP
- Push blood against gravity
- Push fluid out of capillaries into interstitial space (esp in brain arterioles)
- Assure blood can reach the head when standing
- Compliance during aging decreases
- Pulse pressure amplifes w/ aging due to large artery stiffness
Effect of Gravity on CV Control
- Overcoming gravity: greatest challenge that the CV system faces
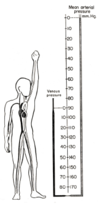
- Normal MAP = 100mmHg = column of blood 4.5 ft high
- BP changes
- BP decreases as blood is propelled upward
- BP increases as blood moves down w/ gravity
- When standing
- Arterial pressure at head = 70mmHg
- Arterial pressure at feet = 170mmHg
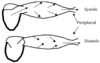
Pressure Waves in Arteries
-
Pressure wave: generated from ejection of blood from the left ventricle
- Felt via palpitation as the periphreal pulse
- Speed of propagation increases w/ increased SV and with decreased arterial compliance
- When pressure wave reaches small peripheral bifurcations, it’s reflected back in the reverse direction
- Distorts arterial wave form to look like greater systolic & pulse pressure in peripheral parteries than in larger proximal arteries
- MAP decreases as the pressure wave propagates as resistance is overcome
Dicrotic Notch / Incisura
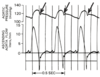
- Aorta absorbs energy during systole and resorbs it during diastole
- In the left ventricle, when it relaxes, BP drops significantly
- Pressure doesn’t drop as rapidly in the aorta as in the left ventricle
- There’s a brief period at the end of systole when blood flows backwards from the aorta in the ventricle
- Triggers closure of the aortic valve and termination of retrograde flow
- Aortic valve opens when pressure in left ventricle > aorta
- Aortic valve closes when pressure in left ventricle < aorta
- Dicrotic Notch / Incisura: discontinuity in the pressure tracing, marker for aortic valve closing
Pressure Waves in Arterioles
- As arteries divide into smaller branches, the amount of connective tissue in the walls diminishes but muscularity increases
-
Arterioles: major resistance vessels, so BP drops when blood flows through them
- As the pressure wave progresses through them, the pulse is almost completely damped out

Law of Laplace
- Describes surface tension and why large arteries contain more connective tissue than small arteries
- T = Pr
- T = wall surface tension
- P = transmural pressure
- r = radius
- Small vessels can sustain a high pressure w/o having a high surface tension and breaking
- Large vessels need a lot of connective tissue reinforcement to sustain pressure since surface tension is high

How blood flows from arterioles to capillaries to venules
-
Capillaries: single layer of endothelial cells + basement membrane
- Thickness of the wall is only ~0.5 micrometers
- Metarterioles: specialized blood vessels that permit large white cells to flow form the arterial to the venous side of circulation
-
Precapillary sphincters: small bands of vascular smooth muscle at the junciton b/n a metarteriole and a capillary
- When contract, they diminish blood flow into capillaries and shunt blood away from capillary beds